“When the recruiter calls, you take the call.” That’s what PriMed Beavercreek primary care physician Dr. Jan Froehlich learned growing up with a father in the Air Force, and that’s why Dr. Froehlich took the call when, as a medical student at the University of Cincinnati in the 1990s, she was offered the opportunity to join the military as part of a health professional scholarship program—in the same branch of the Armed Forces where her father served.
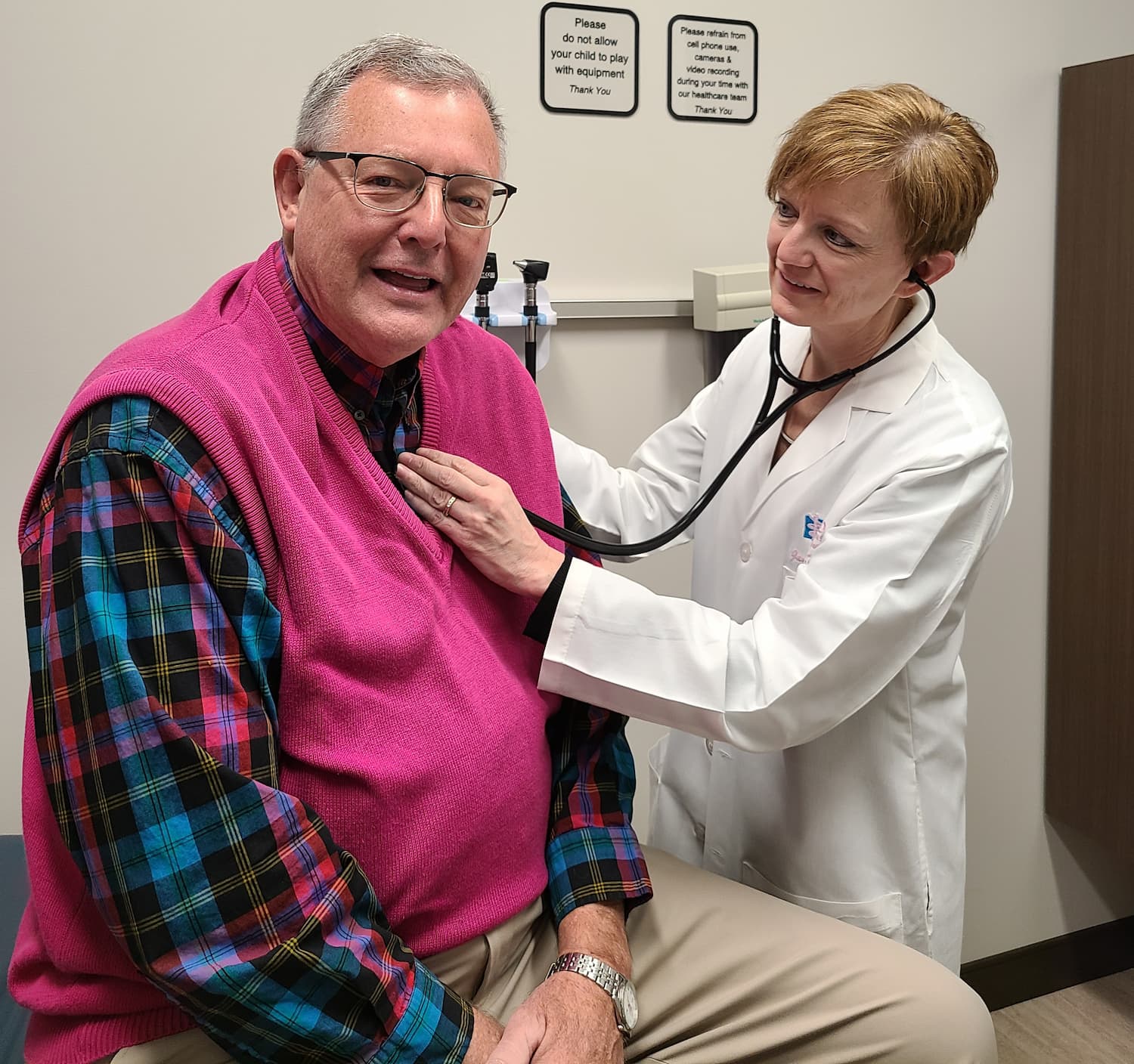
Dr. Jan Froehlich
After serving as a military doctor at Maxwell Air Force Base in Montgomery, Alabama with a dual focus on operational readiness and retiree healthcare, Dr. Froehlich returned to civilian medicine in the Dayton, Ohio, area 17 years ago. Since then, she’s become well-known for her support of senior patients (her practice, PriMed Beavercreek Family Practice, cares for 1,234 Medicare and Medicare Advantage enrollees) while drawing on her background as a military doctor. In honor of Veterans Day, agilon health sat down with Dr. Froehlich to learn more about how value-based care benefits her patients and reflects the values and principles she learned working with military retirees.
Q: What were the most valuable lessons you learned about practicing family medicine in the Armed Forces?
A: Whether military or civilian, a lot of retirement medicine is understanding patients’ lifelong journey through healthcare. I look for things I can use to help guide people to continue their health into their senior years—particularly weight, osteoporosis and chronic-disease management—while delivering consistent, guideline-based healthcare that’s very prescriptive and team-based.
Q: When you began practicing medicine as a civilian, what struck you as the biggest difference from practicing in the Armed Forces?
A: In the Armed Forces, we had a very, very developed pharmacy, but it was limited to only the best and most cost-effective medicines. When you are choosing from three medicines instead of 50, that takes a lot of the noise out of healthcare.
In civilian medicine, oftentimes people come in with ideas of products or therapies they think they need because Facebook or TV told them—for example, things like knee and joint replacements, which aren’t necessarily a needed step. So we now do an osteoarthritis protocol that takes you through the process of using topical agents and Tylenol and Cymbalta, weight loss counseling and physical therapy, and only when you have exhausted all of those options do we now send them to the orthopedist. It’s cost-effective.
Q: How has agilon health supported you in your aim to deliver team-based, compassionate, comprehensive care to your senior patients?
I am very process-driven and that comes from military experience; I don’t need to recreate the wheel. What agilon offers is essentially a team of people who have worked on specific areas and developed best processes that can be employed. I actually take pleasure in employing those in my office because I can take multiple processes and get them rolling for patients instead of just the things that I know most to do. Coming into primary care, I think that’s the only way you can operate because there’s so much depth and breadth you need to cover with any appointment.
Q: How do agilon’s values to transform healthcare through value-based care align with those you learned and practiced in the Armed Forces?
A: In the Armed Forces 17 years ago, the concept of “value-based care” wasn’t there yet, but being able to recognize best processes and practices and feel confident in your colleagues and counterparts, and then being able to employ those processes and practices at your small site, that’s similar to what we did then.
Q: Why do you think moving to a value-based care approach is important for patient care and outcomes?
A: What it does is, it takes healthcare from just the moment of the doctor’s appointment to essentially being part of their life outside of the appointment. In the old days, while a patient was at their appointment, they “got doctored,” and then they went home and did their thing. Today, we do more shared decision-making and they get follow-up support from our staff. Instead of just “doctoring” them when they’re in front of you and then it’s “see you in six months,” we instead allow them to incorporate the healthcare they got at the appointment back into their life. That includes targeting certain patients and saying they need additional care or support.
Q: How do you think PriMed Physicians has embraced this approach?
A: It’s growing every day. Our patients have come to really appreciate and expect now that they get the special touches and they talk to us by name about our team members. It’s everybody working together, not just led by me, and patients feel they are able to reach out and get that support instead of waiting to crash and burn. I appreciate it when people say “I’m Dr. Froehlich’s patient,” but I really like it when they say, “I’m a patient of PriMed Beavercreek.”
Contact for media enquiries
[email protected]Up Next.

Blog Nov 30, 2021 | Article
The Many Ways agilon health is Giving Back
Giving Tuesday is a day when people come together to support their communities through donations ...